About Workforce
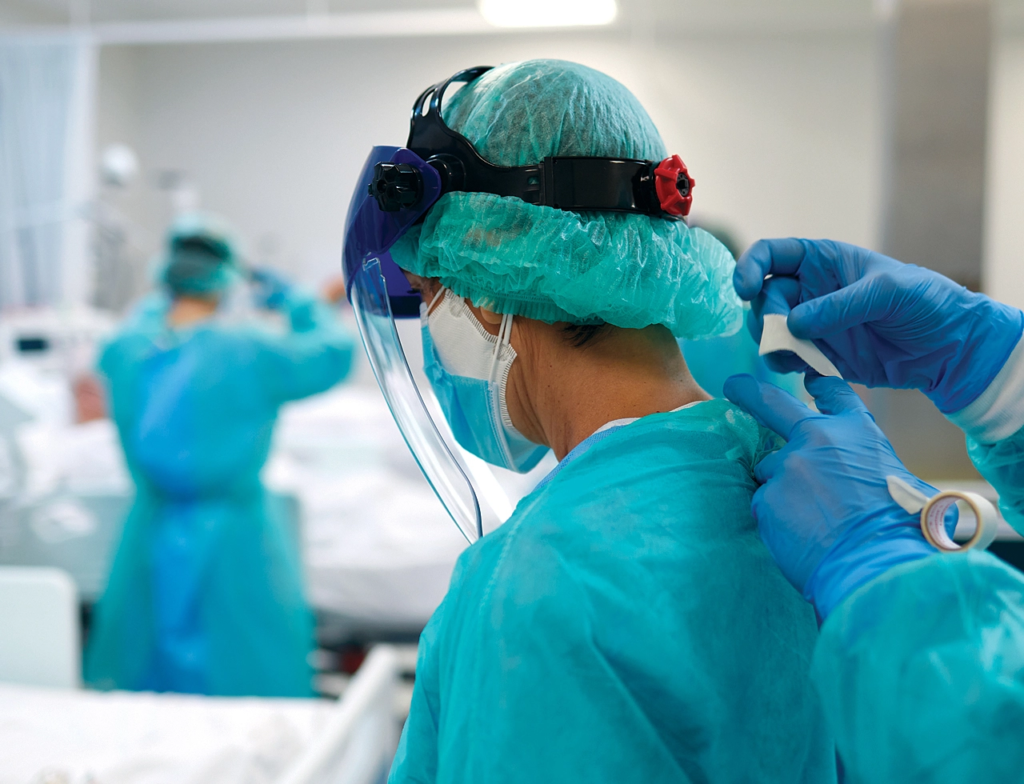
The shortage of health care professionals in California is deepening every year and affects every aspect of care. Statewide, more than 11 million people live in an area without enough primary care providers, and according to a UC San Francisco study of the state’s nursing shortage, it will take until 2026 to close the state’s current nursing gap. All told, California needs to add 500,000 new allied health care professionals by 2024 in order to provide needed care. The COVID-19 pandemic has exacerbated health care staffing shortages. Many front-line health care workers have reached their breaking point and are choosing to leave the profession altogether (hundreds of thousands of health care jobs have been lost since the pandemic began).
Rural and low-income communities are disproportionately affected by the scarcity — and there’s a second disparate impact we must address as the state works to rebuild a depleted workforce: According to the California Future Health Workforce Commission, people of color will be a majority of Californians by 2030 but are severely underrepresented in the health care workforce.
Each year hospitals invest millions of dollars in training California’s next generation of health care providers, but closing the massive gaps ahead will require additional long- and short-term solutions:
- Partnerships among all who recognize the need to protect the health of Californians: employers, workers, policymakers, colleges, licensing entities, and others
- Public investments in workforce training through college and university programs to both retain current workers and build a pipeline of future professionals
- Regulatory changes to improve efficiency and transparency in licensing, address limitations on scope of practice, and enhance education and training for nurses and nurse assistants
5 Things To Know: CalAIM Incentive Payment Plan, Retention Payment Program, Monkeypox Resources
CALAIM INCENTIVE PAYMENT PLAN PROGRAM UPDATE: The California Advancing and Innovating Medi-Cal (CalAIM) Incentive Payment Program is intended to support the implementation and expansion of enhanced care management and community supports by incentivizing managed care plans (MCPs) to drive MCP delivery system investment in provider capacity and delivery system infrastructure. It is also intended to bridge current silos across physical and behavioral health care service delivery; reduce health disparities and promote health equity; achieve improvements in quality performance; and encourage take-up of community supports. More information on the MCP Incentive Payment Plan Program Year 1 Gap Filling Plan is available by county (San Diego and Imperial included) on the Department of Health Care Services website. Additional general information on the Incentive Payment Program can be found on the CalAIM Roundtables by Region web pages for San Diego and Imperial counties.
Hospital Input Needed for Workforce Survey
As hospitals face critical employee shortages, workforce data are essential to providing insight on questions about the supply, demand, and distribution of health professionals.
5 Things To Know: Health Services Task Force, Cybersecurity Project, Health Care Scholarships
HEALTH SERVICES CAPACITY TASK FORCE: The All-Hazard Health Services Capacity Management Plan activation level has been elevated from Level 3 Partial Activation to Level 2 Escalated Activation. Over the last week, system metrics have suggested increasing stresses on health care capacity. These indicators include increased emergency department boarders, larger emergency medical services system volumes, and rising wastewater viral detections. Close system monitoring is ongoing to determine the need to escalate to a higher plan level and various mitigation tools may be activated if necessary. Maintaining masking, physical distancing, and other protective practices are vital to minimizing the level of the current patient surge, and vaccinations and boosters against COVID-19 and influenza are strongly encouraged. The Health Services Capacity Task Force Operational Group continues to meet regularly, and sector representatives will provide important updates, facilitate information sharing, and recommend coordinated plan actions to optimize health care delivery countywide.
5 Things To Know: COVID-19 Rebound After Paxlovid, Workforce Development Grant, Alternatives to Incarceration Report Findings
ALTERNATIVES TO INCARCERATION: On May 24, the San Diego Association of Governments presented its Initial Interim Report on Alternatives to Incarceration to the San Diego County Board of Supervisors. Among some of the findings:
5 Things To Know: Medi-Cal Expansion, HASD&IC Partnership Championed, Youth Drug Webinar
IMPERIAL VALLEY HOMELESSNESS: At the April 12 Imperial County Board of Supervisors meeting, the Imperial Valley Continuum of Care Council Administrative Entity provided details of how they are addressing homelessness and overall accomplishments so far. Updates include a redesign of an operating Coordinated Entry System, the entity’s pandemic response (a region-wide survey to understand needs), update on current continuum of care programs, and projects such as the new Homeless Day Center that will provide services to over 700 individuals per year, Lotus Living Community (transitional housing) for Imperial Valley College students, and youth programs for those experiencing homelessness that have served 156 youth.
5 Things To Know: CalAIM Incentive Program, Monoclonal Antibody Treatments, Resources For Front-Line Staff
MONOCLONAL ANTIBODIES: The California Department of Public Health (CDPH) has issued a COVID-19 Therapeutics Needs Assessment survey to understand how frequently antiviral medications and monoclonal antibody treatments are being used in each jurisdiction and/or health care facility. The survey is designed to help CDPH understand challenges and successes in outpatient treatment of COVID-19. As the landscape of outpatient therapeutics is changing rapidly, there have been several versions of this survey. Hospitals are encouraged to complete the survey even if another version was previously completed. More information on COVID-19 therapeutics options is available on the CDPH COVID-19 treatments page.