About Workforce
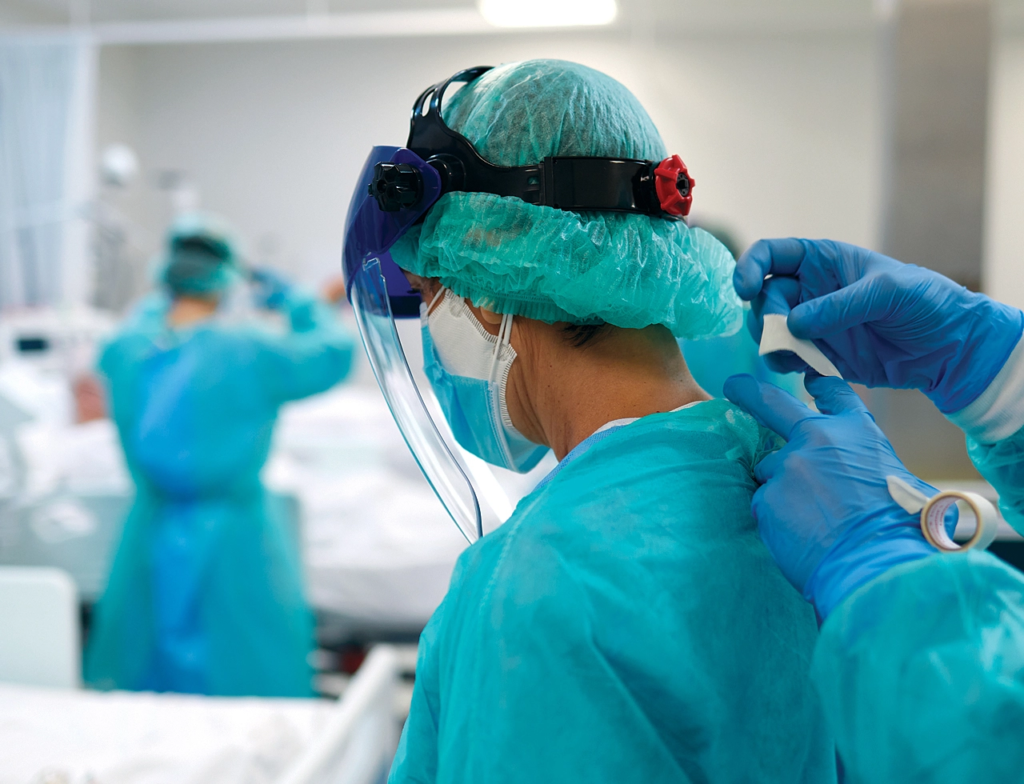
California’s shortage of health care workers is severe. Statewide, more than 22% of Californians live in an area without enough primary care providers. There, patients often face a health care system lacking enough nurses, physicians, pharmacists, and others. California needs to add 500,000 new allied health care professionals such as medical assistants, imaging specialists, and more. Closing the gap will require partnership among employers, workers, policymakers, colleges, licensing entities, and others.
5 Things To Know: Grant Program Seeks Proposals for Addressing Imperial County Health Care Provider Shortage
The County Medical Services Program Governing Board seeks to address the chronic health care provider shortage in its counties — including Imperial County — which it hopes to do via the Building the Healthcare Workforce (BHW) grant program. The board has released a request for proposals for the BHW program, which would support and expand […]
5 Things To Know: HQI Virtual Forum to Discuss Workplace Violence in Critical Access, Rural Hospitals
Individuals leading and supporting hospital efforts to eliminate workplace violence are invited to the next Hospital Quality Institute (HQI) virtual forum on Dec. 12 at noon (PT). The forum will discuss workplace violence concerns and interventions specific to critical access and rural hospitals. Registration is open; questions can be directed to Boris Kalanj, HQI’s director […]
5 Things To Know: Key Workforce Scholarship Deadlines Approaching
The Department of Health Care Access and Information (HCAI) seeks to increase the number of health care providers in underserved communities in California by improving access to health care programs, and is doing so through scholarships, loan repayment, and other training programs for students and graduates. Two key scholarship application deadlines are fast approaching: Dec. […]
5 Things To Know: Save the Date for Primary Care and Behavioral Health Integration Summit
On Jan. 28 and Jan. 30, 2025, from 9 a.m. to 4 p.m. (PT), the 15th annual Primary Care and Behavioral Health Integration Summit — held virtually and at no cost to attendees — will showcase emerging ideas and practices on integrated behavioral health in San Diego County and across the country. Local and national leaders […]
5 Things To Know: HCAI Scholarships Support Students in Health Care Professions
Students can now apply for six different Department of Health Care Access and Information (HCAI) scholarships, which are awarded in exchange for directly a commitment to directly serve patients in a medically underserved community after their education is completed. Designed to support the health care workforce, HCAI offers these scholarships to help students finance education […]
SOHL Leadership Pearls-Population Health: Leading Change & Solutions
The San Diego Organization of Healthcare Leaders’ (SOHL) fourth annual Leadership Pearls event will take place Oct. 23 from 5-8:30 p.m. (PT). SOHL members and the health care community at large are invited to hear from CEOs and senior leaders from San Diego County, who will share their leadership knowledge around population health in the region. Registration […]
5 Things To Know: Health Careers Exploration Program Applications Close Oct. 16
The Health Careers Exploration Program awards a maximum amount of $25,000 to organizations to support conferences, workshops, or career exploration activities that expose students to health careers. The application cycle closes on Oct. 16. An informational webinar was held on Sept. 9, and a recording and additional information are available on the program website.
5 Things To Know: Health Careers Exploration Program Applications Close Oct. 16
The Health Careers Exploration Program awards a maximum amount of $25,000 to organizations to support conferences, workshops, or career exploration activities that expose students to health careers. The application cycle closes on Oct. 16. An informational webinar was held on Sept. 9, and a recording and additional information are available on the program website.
5 Things To Know: HQI to Host Hospital Workplace Violence Virtual Forum
The Hospital Quality Institute (HQI) invites individuals leading and supporting hospital efforts to eliminate workplace violence to register for a virtual forum on Aug. 29 at noon (PT). The event will include discussion on establishing hospital-based programs of peer support aimed at providing emotional first aid to staff who have been affected by workplace violence.
5 Things To Know: CHCF Invites Organizations to Apply for Workforce Initiative
The California Health Care Foundation (CHCF) is inviting organizations to submit a letter of interest for its new Community Health Worker, Promotor, and Community Health Representative Workforce: Community of Practice initiative by Aug. 23. This initiative builds on CHCF’s ongoing efforts to advance these professions in California, reduce health disparities, and increase access to culturally responsive care.