About Workforce
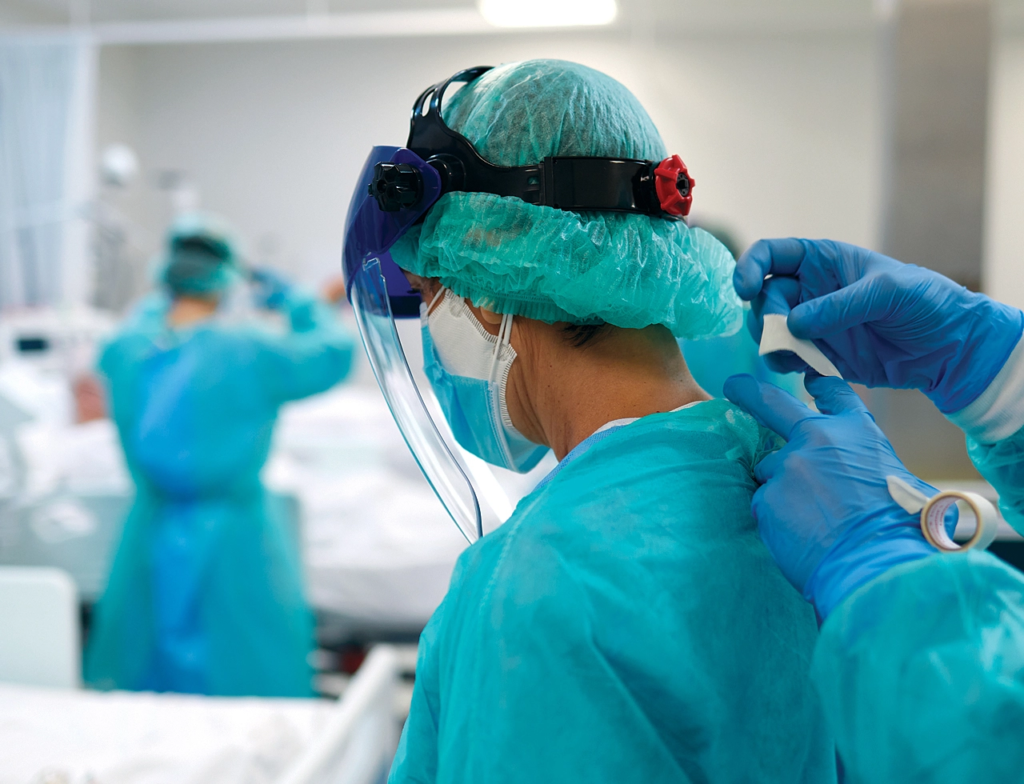
The shortage of health care professionals in California is deepening every year and affects every aspect of care. Statewide, more than 11 million people live in an area without enough primary care providers, and according to a UC San Francisco study of the state’s nursing shortage, it will take until 2026 to close the state’s current nursing gap. All told, California needs to add 500,000 new allied health care professionals by 2024 in order to provide needed care. The COVID-19 pandemic has exacerbated health care staffing shortages. Many front-line health care workers have reached their breaking point and are choosing to leave the profession altogether (hundreds of thousands of health care jobs have been lost since the pandemic began).
Rural and low-income communities are disproportionately affected by the scarcity — and there’s a second disparate impact we must address as the state works to rebuild a depleted workforce: According to the California Future Health Workforce Commission, people of color will be a majority of Californians by 2030 but are severely underrepresented in the health care workforce.
Each year hospitals invest millions of dollars in training California’s next generation of health care providers, but closing the massive gaps ahead will require additional long- and short-term solutions:
- Partnerships among all who recognize the need to protect the health of Californians: employers, workers, policymakers, colleges, licensing entities, and others
- Public investments in workforce training through college and university programs to both retain current workers and build a pipeline of future professionals
- Regulatory changes to improve efficiency and transparency in licensing, address limitations on scope of practice, and enhance education and training for nurses and nurse assistants
Members Encouraged to Enroll in Workforce Survey Program
Attracting and retaining talented employees is a challenge at any time, and the disruption of the pandemic underscores the importance of staying up to date on compensation and human resources trends. To assist hospitals in making informed and strategic hiring decisions, HASD&IC members are asked to enroll in Salarity’s 2022 Allied for Health (AFH) Survey Program by April 1.
5 Things To Know: Workforce Council Meeting, Ambulance Patient Offload Times, Domestic Violence Training
MEDI-CAL MANAGED CARE RFP: On Feb. 9, the Department of Health Care Services (DHCS) released a request for proposal (RFP) for its commercial Medi-Cal managed care plan (MCP) contracts. While this RFP is only for commercial Medi-Cal MCPs, the updated contract will be executed with all Medi-Cal MCPs, including County Organized Health Systems, Local Initiatives, and the new Single Plan Model. The updated MCP contract, which is released with the RFP, also serves as the minimum definition of requirements. MCP proposals are due April 11, and DHCS expects to award contracts to selected plans in August. New contracts will become effective Jan. 1, 2024. A voluntary pre-proposal web conference will be held on Feb. 24 from 1 to 2:30 p.m. (PT). Pre-registration is required, and questions will be taken only via the webinar chat feature.
5 Things To Know: HASD&IC Annual Meeting Donations, COVID Vaccinations by ZIP, Transportation Alternatives
COVID-19 VACCINATIONS BY ZIP CODE: San Diego County’s Weekly COVID-19 Surveillance Report shows the percentage (as of Dec. 4) of the total population of San Diego County residents who are fully vaccinated, by ZIP code of residence. Note that the data only include vaccines that have been recorded in the San Diego Immunization Registry. Some health care providers, including Veteran’s Affairs, the Department of Defense, some tribal entities, and prisons, do not report to the registry.
5 Things To Know: Vaccine Mandates Chart, Children’s Covid-19 Vaccine, Shigella Outbreak
IMPERIAL COUNTY LOCAL HEALTH AUTHORITY: The Local Health Authority Commission met in closed session on Nov. 8 for discussion of current and potential contracting models relating to Knox Keene licensing, pursuant to Welfare and Institutions Code § 14087.38 (m) (n).
5 Things To Know: Medi-Cal RFP Update, Board Meeting Highlights, Key Messaging on Workforce Shortages
MANAGED CARE PLAN RFP UPDATE: The Department of Health Care Services (DHCS) has adjusted the release date of the Medi-Cal Managed Care Plan Request for Proposal (RFP) to Feb. 2, 2022. Although the RFP was scheduled to be released at the end of this year, the change will not affect the implementation date of Jan. 1, 2024. Additional time is needed to address stakeholder comments received during the comment period for the draft RFP. Updates to the RFP schedule will be posted on the DHCS website. HASD&IC will continue to engage with County of San Diego officials on the process. The Imperial County Board of Supervisors has approved the adoption of a single-managed care plan model through an 1115 Waiver.